(512) 377-1744
Introduction
The Merit-based Incentive Payment System (MIPS) is CMS program that works on clinicians payment based on performance across following four areas:
- Quality
- Cost
- Promoting Interoperability
- Improvement Activities
The quality category weighs most in importance. Using measures such as outcomes, processes and high-priority areas, it measures how safe, efficient, and patient focused care your healthcare facility has. Accuracy in reporting is important. It directly affects one’s overall MIPS score, which ultimately determines if they will get a bonus, no change or penalties.

Eligibility and Participation
Who is required to report in 2023
To be able to report under MIPS, you must meet the low-volume threshold, which is based on following criteria:
- At least $90,000 in Part B allowed charges
- At least 200 Part B patients
- At least 200 covered professional services
Clinicians in an Advanced Alternative Payment Model are exempt from MIPS reporting.

MIPS Scoring Framework (2023)
As mentioned earlier, MIPS evaluates providers across four categories. Each category contributes a specific percentage to the final MIPS score, which eventually determines the payment adjustment accordingly for the next year.
Category
In 2023, each category weights were as follows: Quality — 30%, Cost — 30%, Promoting Interoperability—25%, Improvement Activities—15%, All of these percentages apply to clinicians participating in the traditional MIPS.
Performance Threshold for 2023
The performance threshold for 2023 MIPS performance year was set at 75 points total. Providers scoring above this threshold will be eligible for positive payment adjustments, while scoring below it may face penalties.
Payment adjustments
MIPS payment adjustments are based on the final MIPS score, which is calculated by combining the weighted scores from all performance categories. Higher score means bonuses while lower means penalties.
Quality Category 2023
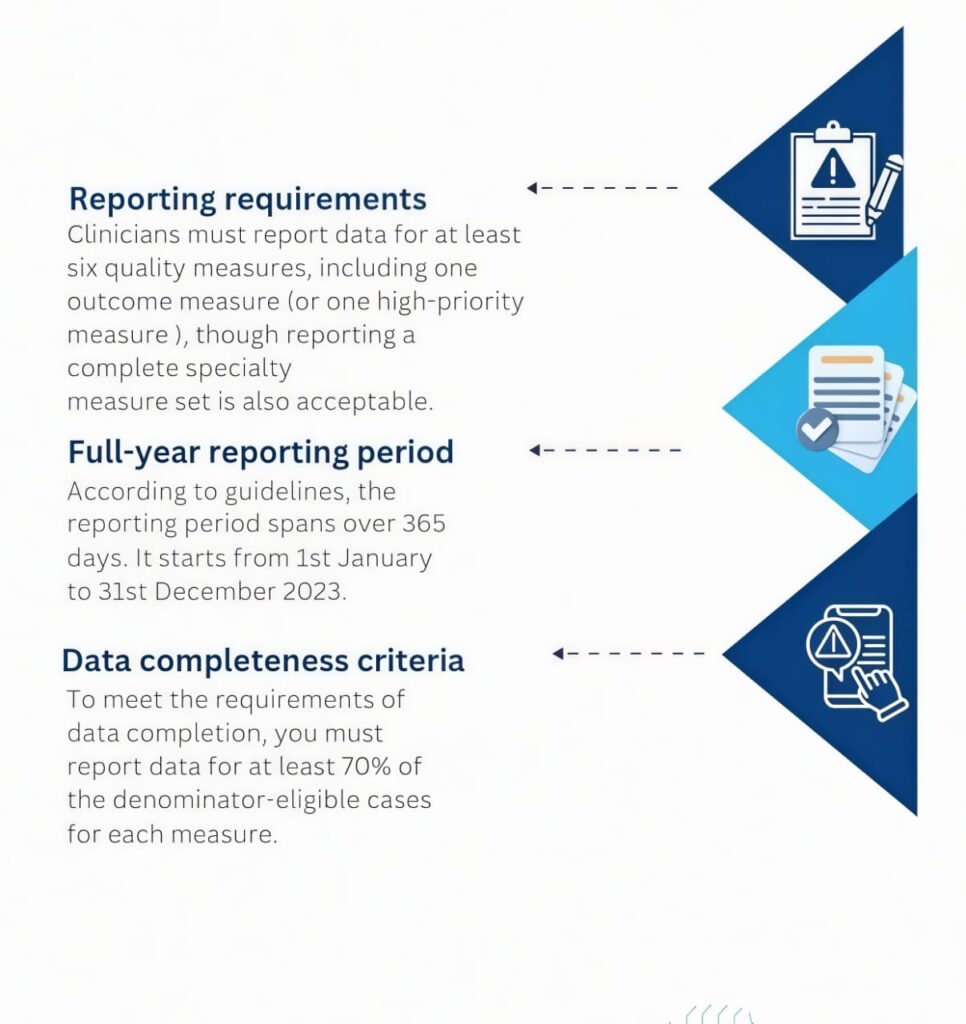

Changes in 2023 Quality Reporting
New measures introduced in 2023
CMS introduced 9 quality measures for the 2023 performance year. These include: 1 administrative claims measure, 1 composite measure, 5 high-priority measures, 2 patient-reported outcomes measures, The purpose of measures is to make quality reporting more complete and useful.
Removed or Retired Measures
In 2023, CMS removed 11 quality measures from the MIPS program. Moreover, 3 measures were partially removed, which means they were removed from traditional MIPS reporting but retained for use in MVPs or Alternative Payment Models.
Updates to existing measures
CMS made changes to 59 existing measures to refine the quality measurement process.
Alignment with MVPs
Starting from 2023, CMS introduced MIPS Value Pathways (MVP) as a new reporting structure. MVP aims to align measures and activities across the quality, cost and improvement activities categories of MIPS. The goal is to make reporting more relevant to a clinician’s practice. This makes reporting easier and performance assessments more meaningful.
Impact of topped-out measures
Measures that nearly everyone already performs perfectly on, called “topped-out” measures, were removed from MIPS. This encourages the creation of more meaningful and challenging measures. CMS tracks the impact on specialty measures and asks stakeholders to develop replacements.
MIPS Values Pathways
Benefits
- Measures focused on provider’s specialty or condition.
- Combines measures across categories, reducing paperwork
- Promotes team work and improves patient outcomes
Challenges
Clinicians must still report promoting interoperability measures, which may need extra attention
- New system may take time to get used to it
- Not all specialties have MVP status available
Key CMS submission portals and tools
According to 2023 quality reporting, all clinicians just submit data in the Quality Payment Program (QPP) website. CMS also offered following tools to make it easier:
- QPP Access Guide: To show how to log in and use the portal.
- Data Submission Guides: Step-by-step instructions for traditional MIPS, MVP, or APM.
- QPP JSON Templates: Ready-made templates for electronic data submission.
Avoiding late submission penalties
To avoid late submission penalties, participants were advised to:
- Submit early
- Check accuracy
- Use CMS resources
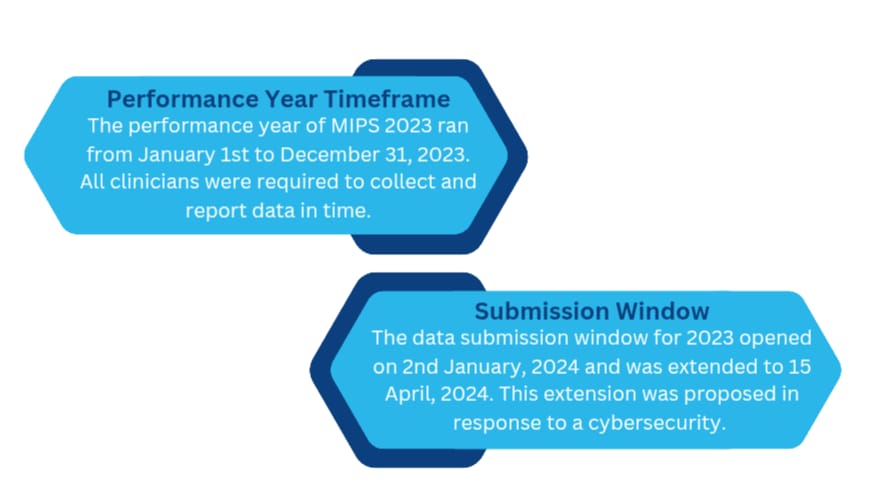

Avoiding Financial Implications In 2023 Reporting
A perfect MIPS score could earn a +2.15% positive adjustments on Medicare payments. Scores below 18.75 points or lower may get a negative adjustment of up to -9%. However, clinicians facing extreme and uncontrollable circumstances are allowed to apply for Extreme and Uncontrollable Circumstances Exception (EUC) to reweight performance categories.
To optimize performance score, following strategies are always advised:
Pick the right measure and match them to your strengths and patients
Track your progress throughout the year
Use CMS tools that can help with accurate reporting
Participate in activities that can earn points and show quality care
Provider burden and reporting complexity
Collecting, checking and then submitting data is time consuming, especially for small practices with limited staff.
Increasing penalties for underperformance
Failing to meet threshold can lead to negative adjustments or penalties up to -9%, which can significantly impact finances of the practice.
Concerns from medical associations
Reporting may take time away from patient care, increase load of administrative work and hit small or rural practices the most.
Impact of frequent measure changes
CMS updates quality measures every year to improve the standard of patient care but it requires practices to quickly adapt and adjust workflows which is a hassle.
Challenges and Concerns


A1 Healthcare
Help Support
Services
Working Hours
- 8AM - 5PM
- Central Standard Time
- Monday - Friday
